Here's Why Your Local ER Faces More Visits Each Year
Emergency rooms (ERs) are experiencing a notable increase in the number of visits each year across the country, a trend that demands our attention. According to Becker's Hospital Review, in Texas, there are 49 emergency department visits per 100 people annually. As the frontline of healthcare, ERs are crucial for handling urgent medical situations, yet the rising tide of visits stretches their capabilities. This blog delves into various contributing factors that are making ERs busier than ever. By examining demographic shifts, healthcare system constraints, increasing chronic diseases, and socio-economic challenges, we aim to offer a comprehensive understanding of this complex issue.
The Aging Population
Growing Number of Elderly Individuals
The aging population is a significant driver of the increase in local ER visits. As people age, they become more susceptible to health issues, requiring frequent medical interventions. The baby boomer generation is now entering retirement age, resulting in a larger elderly population than ever before. This demographic shift brings about a greater demand for healthcare services, including emergency care. The necessity for specialized geriatric care in ERs also rises, which can strain resources designed for acute and critical conditions.
Increased Prevalence of Chronic Diseases
Furthermore, chronic diseases are a hallmark of aging, contributing to the surge in local ER visits. Conditions such as hypertension, diabetes, and heart disease become more prevalent with age, often necessitating immediate attention. Seniors with chronic illnesses frequently face health crises that warrant emergency intervention. This prevalence is exacerbated by lifestyle factors that compound the severity of these diseases. The management of chronic conditions often lacks adequate support in outpatient settings, leading seniors to seek aid from ERs as a first line of defense.
Higher Risk of Injuries and Accidents
With age comes a heightened risk of injury and accidents, such as falls, which frequently lead to ER visits. Elderly individuals are particularly vulnerable to falls due to factors like decreased mobility and balance. These incidents can result in serious injuries, like fractures, which require urgent medical attention. The injuries sustained often necessitate advanced imaging and diagnostic services available in ERs. Consequently, emergency departments increasingly act as primary responders to accidents involving older adults.
Limited Access to Primary Care for Seniors
Access to primary care remains a persistent challenge for seniors, contributing to higher local ER utilization. Many elderly individuals face barriers such as transportation issues, making it difficult to attend regular medical appointments. There is also a shortage of geriatric specialists and primary care providers, leading to delayed diagnoses and management. This scarcity compels seniors to rely on ERs for conditions that could have been managed in outpatient settings. The limited availability of after-hours care further drives elderly patients to emergency services.
Shortage of Primary Care Providers
Decrease in General Practitioners
The shortage of primary care providers is a critical issue that drives more people to ERs. Over the years, the number of general practitioners has not kept pace with the growing population, leading to a significant gap in healthcare provision. Medical students often choose specialties over general practice, drawn by greater financial incentives and prestige. This trend results in fewer doctors available to manage day-to-day healthcare needs. Consequently, patients without a primary care provider often turn to ERs for healthcare needs that do not necessarily require emergency interventions.
Longer Waiting Times for Appointments
With fewer general practitioners available, patients experience longer waiting times for appointments. This delay can be critical, especially for conditions that could deteriorate without timely intervention. For many patients, the wait can stretch from weeks to months, depending on severity and location. Long waits discourage patients from seeking help in primary care settings, pushing them towards ERs where service is perceived as immediate. This reliance on emergency facilities for situational healthcare stems from systemic inefficiencies that restrict patient access to timely care.
Overburdened Clinic Environments
Primary care clinics are often overburdened, which impacts the quality of care and accessibility for patients. High patient-to-doctor ratios limit the time doctors can spend on individual cases, potentially overlooking crucial health issues. The high volume of patients leads to rushed consultations and the possibility of incomplete evaluations. This situation drives individuals to seek comprehensive treatment in ERs, where more time and technological resources are available. Overburdened clinics inadvertently direct patient flow towards emergency departments.
Patients Seeking Immediate Care in ERs
Additionally, ERs provide the promise of immediate care, making them an attractive option for individuals seeking quick medical attention. The promise of speed and comprehensive diagnostics compels patients to opt for emergency services instead of enduring long waiting periods at clinics. In cases of acute pain or sudden worsening of conditions, patients may view ERs as their only option. However, this surge in patient flow increases wait times in ERs themselves, sometimes leading to treatment delays. The preference for immediate care underscores systemic issues in healthcare delivery that need addressing.
Increased Prevalence of Chronic Conditions
Rise in Diabetes and Obesity Rates
Chronic conditions like diabetes and obesity are on the rise, significantly influencing local ER visits. These health issues are often exacerbated by lifestyle choices and socio-economic factors, leading to urgent medical situations. Diabetes-related emergencies, such as hypoglycemic events, require timely intervention, commonly found in ERs. Similarly, obesity heightens the risk for ailments like heart disease that might necessitate emergency care. Public health initiatives focusing on lifestyle modifications may help reduce the burden on ER resources over time.
Heart Disease in Emergency Settings
Heart disease remains a leading cause of emergency room visits, requiring specialized emergency management. Episodes like heart attacks demand immediate attention, pushing patients to seek local ER services where rapid response teams are available. Modern ER facilities are equipped with technologies for diagnosing and managing cardiac emergencies, making them vital for acute situations. However, the lack of consistent outpatient care often means these conditions reach a crisis point before intervention occurs. Balancing emergency responses with preventive heart health measures is necessary to control visit frequency.
Asthma and Respiratory Emergencies
Respiratory conditions like asthma present frequent emergencies that necessitate ER visits. Environmental factors exacerbate these conditions, leading to difficulties that require immediate treatment. ERs offer critical care for asthma attacks, particularly when other healthcare options are inaccessible. Immediate interventions for respiratory distress provide invaluable temporary relief but don't address the underlying causes. The increasing incidence of respiratory issues highlights the need for comprehensive, ongoing management outside of emergency settings.
Mental Health Episodes Leading to ER Visits
Mental health crises increasingly contribute to the increased footprint in ER visits. Patients experiencing severe episodes or suicidal thoughts are often brought to emergency departments for stabilization. The ER becomes an immediate intervention point due to the insufficiency of outpatient mental health services. Emergency care providers often manage these crises with limited psychiatric resources, reflecting the broader shortcomings in mental health support systems. Broadening mental health services beyond ERs could substantially lower visit rates.
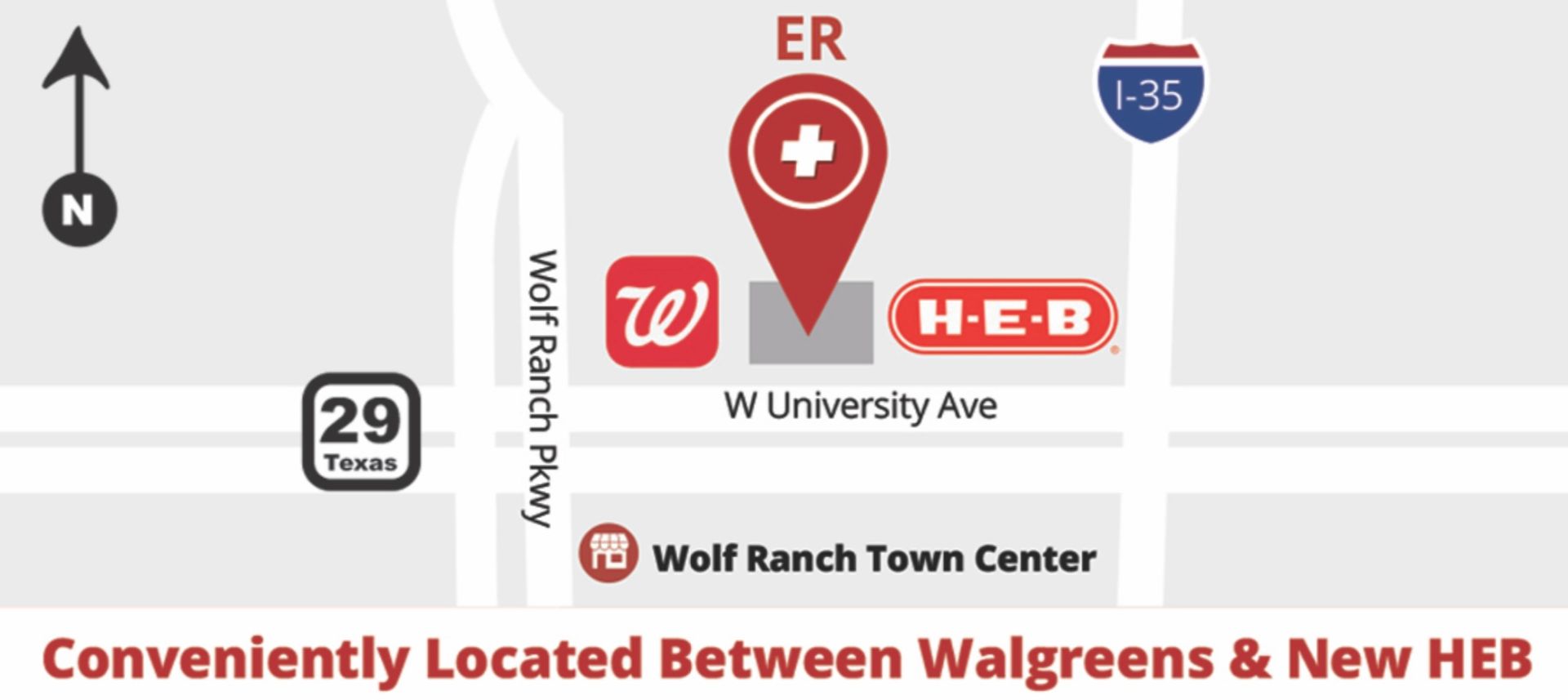
The multifaceted rise in emergency room visits is driven by several interlinked causes, from an aging population and chronic diseases to systemic healthcare shortages and socio-economic challenges. The increasing prevalence of chronic conditions, clinical access limitations, and broader public health crises all contribute to the escalating demands on ERs. If you need a local ER or would like more information, contact us today at Family Emergency Room at Georgetown.

















Share On: